
Medicare is a lot of things, but it isn't always clear.
Specifically, it isn't always clear which kinds of medical equipment and supplies the program does and doesn't cover.
For example, does Medicare cover blood glucose meters or blood pressure monitors? Or does Medicare cover hospital beds, walkers, wheelchairs, or scooters?
Don't feel bad if you have no idea whether or not Medicare helps enrollees pay for those pieces of equipment. You'll be fully educated on the subject by the time you finish reading this article.
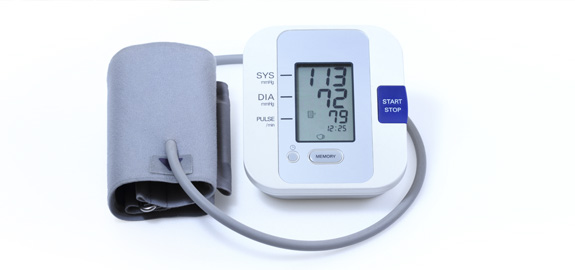
Blood Pressure Monitors
What is a blood pressure monitor? Why do people need blood pressure monitors?
The kind of blood pressure monitor we're talking about here allows people to check or measure their blood pressure from the comfort of their own homes. This is important if you're diagnosed with hypertension, or high blood pressure. It also can be important if you suffer from “white coat syndrome.” People with this condition tend to have above-normal blood pressure readings when they're taken in a doctor's office or clinical environment, but not in other settings and situations. At-home blood pressure monitors, also known as “ambulatory blood pressure monitoring" (or ABPM) devices, let both groups of individuals track these readings without having to make regular trips to see their physicians.
Does Medicare cover blood pressure monitors?
In some cases, yes, Medicare helps people buy or rent blood pressure monitors or ABPM devices so they can keep an eye on their blood pressure readings. Which cases? One example or exception is when someone needs to receive blood dialysis at home. Another is when a Medicare enrollee is diagnosed--after repeated in-office and out-of-office testing--with the above-mentioned “white coat syndrome" and shows no evidence of end-organ damage.
How does Medicare cover blood pressure monitors?
If you fit into one of the categories mentioned in the last section, Medicare should cover part of the purchase or rental cost of an at-home blood pressure monitor. Specifically, Medicare Part B will pay 80 percent of the Medicare-approved amount for one of these devices. You will be responsible for the remaining 20 percent of the bill.
Keep in mind: Medicare only covers these and other devices--often called "durable medical equipment," or DME--if you buy or rent them from suppliers that are enrolled in Medicare. If the supplier you use isn't enrolled, Medicare won’t pay the claim it submits. As such, ask suppliers if they're enrolled in Medicare before you buy a blood pressure monitor from them. Also ask if they're "participating suppliers." Suppliers that are enrolled in Medicare but aren’t “participating" may not accept assignment, and suppliers that don't accept assignment can charge what they want for a product. In those situations, you'll have to pay the difference between the Medicare-approved amount and the amount the supplier charges.
What about Medicare Advantage plans--do they cover blood pressure monitors?
As you may know, especially if you've read our read our "Guide to Medicare Advantage Plans," Medicare Advantage plans, also known as Medicare Part C, must cover pretty much everything Original Medicare (or Medicare Part A and Part B) covers. Well, some Medicare Advantage plans expand that coverage to include things like at-home blood pressure monitors, too. To find out if your plan provides this extra coverage, contact the company that sold it to you.

Blood Sugar Monitors, Test Strips, and Other Diabetes Supplies
What is a blood sugar monitor? What are test strips? Why do people need blood sugar monitors and test strips?
Blood sugar monitors, or blood glucose meters, let people with diabetes measure the amount of sugar (glucose) in their blood and thus manage the disease. Those same people use test strips to obtain blood glucose readings from their blood sugar monitors.
Test strips may soon be a thing of the past, by the way. Late last year, the U.S. Food and Drug Administration (FDA) approved the first continuous glucose monitoring system that doesn't require people to draw blood several times a day. The question is: will Medicare cover these new devices like it currently covers traditional blood sugar monitors and blood glucose meters?
Does Medicare cover blood sugar monitors and test strips?
If your doctor or physician diagnoses you with diabetes and prescribes a blood sugar testing monitor so you can stay on top of the disease, Medicare Part B should help you pay for it. It also should help you pay for test strips and some other supplies.
How does Medicare cover blood sugar monitors and test strips?
Medicare covers blood glucose meters and test strips in the same way it covers blood pressure monitors and other DMEs. In other words, you pay 20 percent of the Medicare-approved amount (as well as the Part B deductible) and Medicare pays the rest.
This is true whether you buy or rent your blood sugar monitor--as long as the supplier you to use buy or rent the device is enrolled in Medicare, of course. If it isn't, you'll be responsible for the whole bill.
Does Medicare cover any other devices or supplies that help treat diabetes?
Yes, Medicare Part B also covers these diabetes supplies:
- insulin
- lancets and lancet devices
- blood sugar control solutions (used to check test strip and monitor accuracy)
- therapeutic shoes or inserts
Note: you may need to use specific suppliers to buy some of the above.
Medicare Part B also covers these diabetes services:
- diabetes self-management training
- yearly eye exams
- foot exams
- glaucoma tests
- nutrition therapy services
Canes, Walkers, and Rollators
Does Medicare cover canes or walkers?
Medicare lumps canes, walkers, and rollators--rolling walkers, basically--in with blood pressure monitors and blood glucose meters as examples of durable medical equipment. And since Medicare (Part B) covers both blood pressure monitors and blood glucose meters, it probably shouldn't be a surprise to hear it covers canes, walkers, and rollators, too.
Medicare doesn't cover all canes, however. Specifically, it doesn't cover white canes for the blind, for whatever reason.
As is true of most other DMEs, Medicare only covers canes, walkers, or rollators that a doctor or other care provider prescribes. Also, you have to a buy or rent these pieces of equipment from Medicare-certified suppliers if you want the government to pick up some of the resulting bill.
How does Medicare cover canes or walkers?
Once again, if you meet the criteria mentioned above (your doctor prescribes your cane, walker or rollator, and you rent or buy it from a participating supplier), your Part B coverage will pay for 80 percent of the Medicare-approved amount. You will pay the remaining 20 percent as well as whatever's left of your Part B deductible.
Do you have a Medicare Supplement--or MedSup or Medigap--plan? It may cover some or all of your portion of this bill. It may cover other, related out-of-pocket costs Medicare Part A and Part B won't cover, too. Want to know more? See our "Medicare Supplement Insurance Policy FAQ."

Hearing Aids
Does Medicare cover hearing aids?
Although Original Medicare doesn't cover routine hearing exams, it does cover hearing exams a doctor considers medically necessary. It also covers cochlear implants--when they're medically necessary, naturally.
Surely that means Medicare covers hearing aids, too, right? Wrong. For that, you need Medicare Part C, or Medicare Advantage.
Not only do Medicare Advantage plans, sold by private insurance companies that have contracted with Medicare, cover pretty much everything Medicare Parts A and B cover, but some expand that coverage to include things like routine hearing exams and even hearing aids.
To learn more about these policies, read our "Guide to Medicare Advantage Plans." When you're done, check out our article about health insurance and hearing care coverage.
How do Medicare Advantage plans cover hearing aids?
It's impossible to say, as one Medicare Advantage plan can be very different from another.
Regardless, you'll probably have to pay both a deductible and a copayment before your Medicare Advantage plan will kick in its share.
To find out for sure if your Medicare Advantage plan covers hearing aids and how it covers them, contact the company that sold it to you.
Hospital Beds
What is a hospital bed? And why do people need hospital beds in their homes?
Hospital beds are exactly what you think they are--they're the type of bed you'd lay and sleep on if you were admitted into the hospital. Typically, they're the same width as a twin bed but a bit longer in length. Most allow you to manually or electronically elevate a person's head or feet, and they also let you adjust the overall height of the bed in the same way. Some feature railings, trapeze bars, IV poles, and bedpans, too.
As for why a person might want to have a hospital bed at home, the main reason is that some people need the specific kinds of support they provide. For example, some need side railings to keep them from falling out of bed, or they need the railings for support. The same is true of the trapeze bars mentioned earlier, which help people reposition themselves. Being able to raise and lower the bed in various ways can be helpful, too.
Does Medicare cover hospital beds for home use?
If your doctor or physician considers a hospital bed medically necessary and prescribes one for home use, your Medicare Part B coverage will help pay for it.
Actually your Part B coverage will help you pay for a manual-lift hospital bed. It won't help you pay for a full-electric model. If you want the latter, you can pay the difference between the two out of your own pocket.
Medicare will help pay for some needed accessories, too, such as trapeze bars, mattress covers, and bedside rails.
And of course you should be able to rent, rather than buy, a hospital bed and still benefit from Medicare's assistance.
Lift Chairs and Stair Lifts
What is a lift chair? What is a stair lift? Why do people need lift chairs or stair lifts in their homes?
A lift chair, sometimes called a "seat lift chair," is a chair with a motorized device attached to it that helps the person sitting on it stand up. It also can help a person who is standing sit down.
A stair lift, on the other hand, is a chair that's attached to a staircase--usually using rails and screws--and lets the person sitting on it ride from one floor or level of a house to another.
Why do people need to bring or install these devices in their homes? The main reason people buy lift chairs is they need assistance standing or sitting. As for stair lifts, they help people who have depth-perception issues, visual problems, or various physical impairments safely move about a home.
Does Medicare cover lift chairs? Does Medicare cover stair lifts?
Medicare.gov is strangely unhelpful when it comes to the subject of lift chairs and stair lifts. Although this page says Part B covers "patient lifts" in certain situations, it doesn't offer up any additional details. That's a problem, as most people think of patient lifts as being devices that help transfer people to and from a bed or wheelchair.
Still, other sources suggest Medicare does sometimes cover part of the cost of buying or renting a lift chair or stair lift. In the case of the lift chair, for instance, Part B (or Part C, Medicare Advantage) may help you pay for the seat-lift mechanism but not the chair itself. Part B may help you pay for a portion of a stair lift, too, but don't expect too much assistance here. At most, it could cover an elevating seat that makes it easier, and safer, for the rider to sit down and get up from the chair.
Portable Oxygen Concentrators and Accessories
What is a portable oxygen concentrator? Why do people need portable oxygen concentrators in their homes?
A portable oxygen concentrator is a device that lets people treat various diseases via oxygen therapy while on the go.
Some of the short-term diseases people treat with portable oxygen concentrators: asthma flare-ups, pneumonia, and respiratory distress syndrome.
People also treat these long-term diseases with portable oxygen concentrators: Chronic Obstructive Pulmonary Disease (COPD), cystic fibrosis, late-stage heart failure, and even sleep apnea.
Does Medicare cover portable oxygen concentrators?
Medicare Part B covers either the rental or purchase of both oxygen equipment and accessories--such as containers that store oxygen and tubing that delivers it--if a doctor or physician prescribes them for use at home.
You also have to meet these conditions to earn Medicare's assistance:
- your doctor says you have a severe lung disease or you’re not getting enough oxygen
- your health might improve with oxygen therapy
- your arterial blood gas level falls within a certain range
- other alternative measures have failed
By the way, Part B also pays for humidifiers when they're used with oxygen equipment.
Scooters and Wheelchairs
Does Medicare cover scooters? Does Medicare cover wheelchairs?
This one's easy. Medicare considers both wheelchairs, even power-operated ones, and scooters to be durable medical equipment. Given that, do you think Medicare covers them? If you answered "yes," pat yourself on the back, because you're right.
Before you run out and buy either a power-operated wheelchair or scooter for yourself, though, you should know that Medicare makes you jump through the following hoops before it'll contribute to the cost of the device.
- First, you have to see your doctor or physician and get him or her to declare that you need a scooter or wheelchair for medical reasons.
- For that to happen, you'll likely need to have a health condition that makes it difficult for you to move around in your home.
- Also, you must be unable to do various activities of daily living--such as bathing, dressing, or getting in or out of a bed or chair--even with the help of a cane or walker.
- You must be able to get on and off the scooters or wheelchair and to safely operate it as well.
- With that out of the way, all that's left is for your care provider--doctor or physician--to submit a written order to Medicare explaining why you need the wheelchair or scooter and that you can safely operate it.
How does Medicare cover scooters and wheelchairs?
Like it does with almost all other DMEs, Medicare will pay 80 percent of the approved amount of your wheelchair or scooter purchase. You will pay your Part B deductible and then 20 percent of the approved amount.
If you have a MedSup or Medigap plan, it may help you pay some of your portion of this bill. Look at your policy documentation or contact the company that sold you this coverage to find out if this is the case or not.
Pick up the phone or send an email to your insurer, too, if you have a Medicare Advantage plan. It may require you to take different steps than the ones mentioned above or to use specific suppliers to buy your new scooter or wheelchair.
Finally, you don't have to buy your wheelchair or scooter. You can rent it instead. This could save you a lot of money, especially if you don't think you'll need the device for very long.
Fraud and Medicare Coverage of Medical Devices and Supplies
Contact Medicare if a supplier offers to:
- give you a “free” wheelchair or scooter
- pay you cash or waive your copayment
- have a doctor you don’t know prescribe you a scooter or wheelchair
All of the above are common examples of fraud connected to Medicare coverage of medical devices and supplies.
A few others:
- a supplier calls you and asks you for your Medicare number, your Social Security Number, or your bank account or credit card information
- you believe Medicare is being charged device, supply, or service you didn’t receive
- you don’t know the physician or supplier named on your Medicare claim
Frequently Asked Questions
Q: What determines if something is a piece of durable medical equipment?
A: According to Medicare.gov, all covered DMEs are:
- durable (they can withstand repeated use)
- used for a medical reason
- used in the home
- not usually useful to someone who isn't either sick or injured
Also, Medicare expects the DMEs it covers to last at least three years.
Q: Medicare told me I have to use a "participating supplier" if I want my device to be covered. What does that mean?
A: As mentioned earlier, Medicare only covers the devices and products discussed in this article if you buy or rent them from suppliers that are enrolled in Medicare. If you use a supplier that isn't enrolled, Medicare won’t pay the claim the company submits.
Because of this, make sure you ask suppliers if they're enrolled in Medicare before you buy devices or other products from them. And ask if they're "participating suppliers," too. Suppliers that enroll in Medicare but aren’t “participating" may not accept assignment, and suppliers that don't accept assignment can charge what they want for a product.
If you buy something from a supplier that doesn't accept assignment and it charges more than the Medicare-approved amount, you'll need to pay the difference out of your own pocket.
Q: Where can I buy medical equipment or devices that Medicare will cover?
A: If you need any help in this area, ask with your doctor or physician. Another option is to contact Medicare and talk with someone there. Or you can head to medicare.gov/supplierdirectory/search.html. After you enter your ZIP code in the search field in the upper-left corner of the screen and you select the categories you're interested in, you'll be shown a list of suppliers in your area.
References:
QuoteWizard.com LLC has made every effort to ensure that the information on this site is correct, but we cannot guarantee that it is free of inaccuracies, errors, or omissions. All content and services provided on or through this site are provided "as is" and "as available" for use. QuoteWizard.com LLC makes no representations or warranties of any kind, express or implied, as to the operation of this site or to the information, content, materials, or products included on this site. You expressly agree that your use of this site is at your sole risk.
View Medicare Disclosure
QuoteWizard is owned and operated by QuoteWizard.com, LLC (“QuoteWizard”), a subsidiary of LendingTree, LLC. Copyright © QuoteWizard Insurance Solutions, LLC. All rights reserved. Invitations for application for insurance may be made through QW Insurance Solutions, LLC (“QWIS”), a subsidiary of QuoteWizard, or through its designated agents, only where licensed and appointed. Licensing information for QWIS can be found here. QWIS is a non-government licensed health insurance agency. Not affiliated with or endorsed by any government agency. Callers will be directed to a licensed and certified representative of Medicare Supplement insurance and/or Medicare Advantage HMO, HMO SNP, PPO SNP and PFFS organizations. Your call will be routed to a licensed agent who can provide you with further information about the insurance plans offered by one or more of our third-party partners. Each of the organizations they represent has a Medicare contract. Enrollment in any plan depends on contract renewal. Availability of benefits and plans varies by carrier and location and may be limited to certain times of the year unless you qualify for a Special Enrollment Period. We do not offer every plan available in your area. Any information we provide is limited to those plans we do offer in your area. Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options. Deductibles, copays, coinsurance, limitations, and exclusions may apply. Medicare has neither reviewed nor endorsed the information contained on this website.